The Program
Screening Service
Organisation of the Screening Service
Approximately 11 Million women in Germany between the ages of 50 and 69 are eligible for biennial mammography screening. The Screening service is financed by the health insurance funds (statutory and private) and free of charge for the women using it (exceptions may exist for certain individual contracts with private insurances).
Every 24 months, each eligible woman receives a letter from her regional invitation center suggesting a date and a time for an appointment at her assigned mammography unit. The Date and time can be changed personally by contacting the invitation center. Also, women can generally refuse the invitation.
The written invitation also contains a decision aid with balanced, evidence-based information about the benefits and harm resulting from mammography screening. In addition, before having the mammogram, women can make an appointment for personal discussion with a screening physician.
Decision aid provided by the Federal Joint Committee
 MAMMOGRAPHY SCREENING A Decision Aid
(pdf 1.1 MB)
MAMMOGRAPHY SCREENING A Decision Aid
(pdf 1.1 MB)
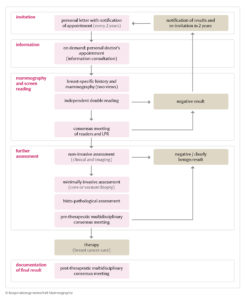
The screening service is provided in certified screening units by specialized personnel. It follows a given protocol displayed in Figure 3.
In the mammography unit, the woman answers a standardized questionnaire concerning her patient breast-specific history. A radiographer carries out the screening mammograms. Two X-ray images are taken of each breast from two different views (mlo=mediolateral-oblique and cc=craniocaudal).
Independent double reading is guaranteed for each mammogram. In case of suspicious findings by at least one of the readers, the mammogram is discussed in a consensus meeting held by both readers together with the lead program radiologist. The result of the consensus meeting is either a normal, or benign, finding or an indication for further assessment is needed. In the latter case, the woman is recalled within a week. In both cases, information on screening results is sent to the women within 7 working days of the screening appointment.
Assessment is conducted in two steps. First, a clinical examination and further imaging is used for diagnostics. If the lesion is assessed as suspicious, histopathological diagnosis is carried out by means of core needle or vacuum-assisted breast biopsy. Histopathological results of biopsies are discussed in a weekly pre-therapeutic multidisciplinary meeting.
If cancer is diagnosed, the woman is referred to a breast cancer center for treatment (not part of the screening-program). After surgical treatment, each case is discussed again, and pathology results are documented in a post-surgical multidisciplinary meeting in the screening unit.
Quality Management
The quality requirements for the German breast cancer screening program are based on the European Guidelines for Quality Assurance in Breast Cancer Screening and Diagnosis (4th edition).
An overview of the quality management system is provided in Figure 4.
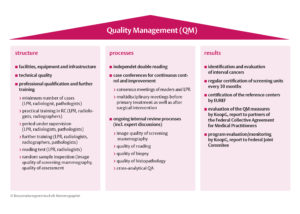
Figure 4: Quality management system of the breast cancer screening program (LPR) – lead program radiologist, RC – reference center)
Certification
To ensure a high level of quality and economic efficiency, the screening service is provided within specialized and licensed facilities – the screening units. The lead program radiologists are selected by public tender for a predefined region. Both certification and regular re-certifications are carried out by KoopG and the relevant reference center by order of the regional Association of Statutory Health Insurance Physicians (ASHIP). Certification and re-certification procedures check that all requirements stipulated by the screening directives are met, including the professional qualification of screening personnel, the physico-technical requirements of the equipment, the performance of the screening service, the implementation of quality management, and the results of performance indicators for the screening unit. The entire process to establish screening service in a defined area is depicted in Figure 5.